Introduction
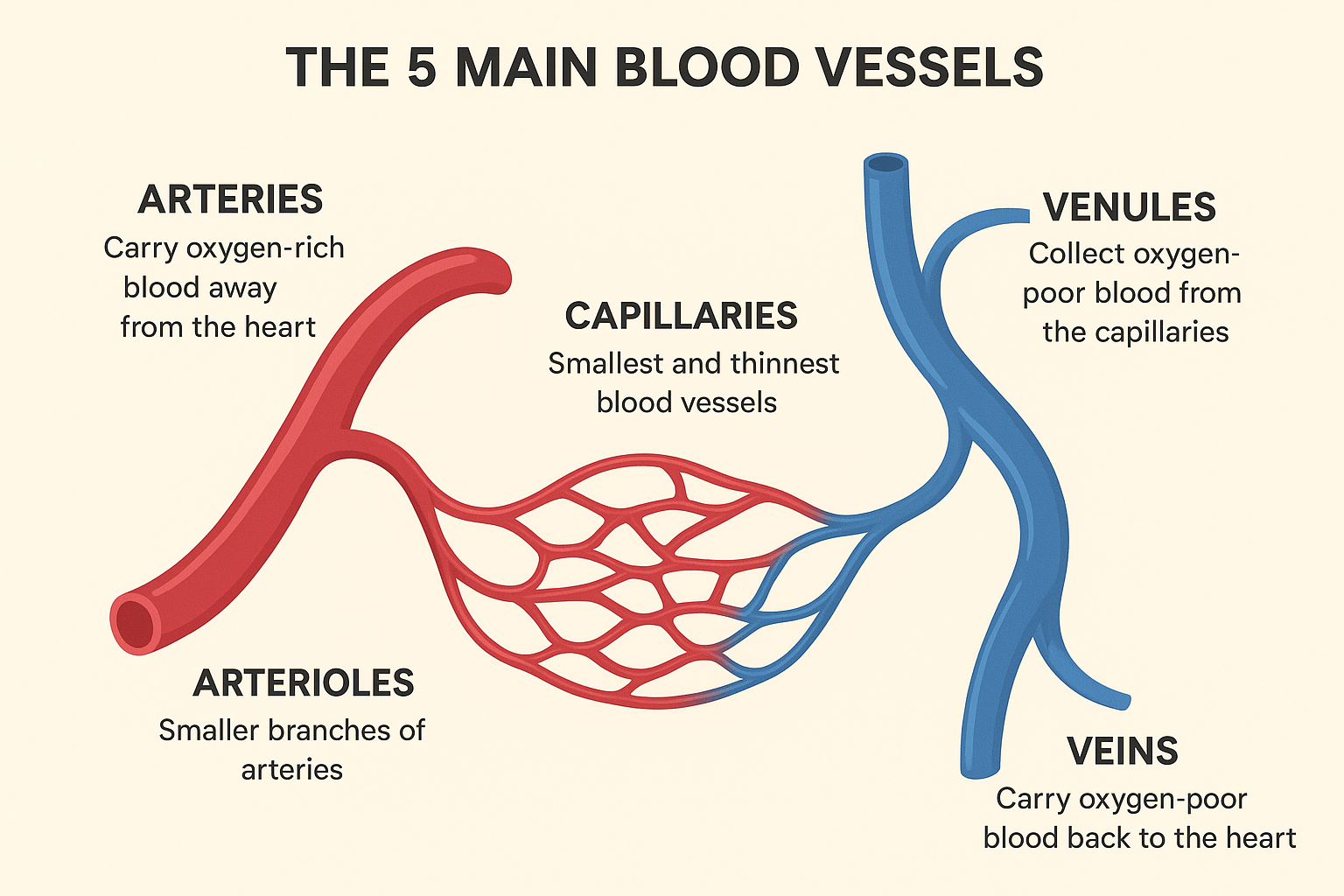
The human circulatory system is a complex network of organs and blood vessels that transports blood, nutrients, oxygen, carbon dioxide, and hormones throughout the body. This vital system is essential for maintaining homeostasis and ensuring the proper functioning of all bodily systems. At the heart of this intricate network are the blood vessels, which act as the pathways for blood flow. While there are numerous types of blood vessels, five main categories play distinct and crucial roles: arteries, veins, capillaries, the aorta, and the pulmonary arteries and veins. This article will delve into the anatomy, function, and clinical significance of each of these primary blood vessels, highlighting their importance in the overall cardiovascular system.
1. Arteries: The High-Pressure Pipelines
Arteries are robust, muscular blood vessels that carry oxygenated blood away from the heart to the rest of the body. They are the high-pressure pipelines of the circulatory system, designed to withstand the powerful force of blood being pumped from the heart. The arterial system begins with the aorta, the largest artery, and branches into progressively smaller vessels, eventually leading to arterioles, which then connect to the capillary network.
Anatomy of Arteries
The walls of arteries are composed of three distinct layers:
•Tunica Intima: The innermost layer, consisting of a smooth endothelium that allows blood to flow with minimal friction.
•Tunica Media: The middle layer, which is the thickest and most muscular. It is composed of smooth muscle and elastic fibers, which allow the artery to expand and contract with each heartbeat. This elasticity is crucial for maintaining blood pressure and ensuring a continuous flow of blood.
•Tunica Externa (Adventitia): The outermost layer, composed of connective tissue that provides structural support and anchors the artery to surrounding tissues.
Function of Arteries
The primary function of arteries is to transport oxygen-rich blood from the heart to the body’s tissues. The muscular and elastic nature of arterial walls allows them to play an active role in regulating blood pressure and flow. When the heart contracts (systole), the arteries expand to accommodate the surge of blood. When the heart relaxes (diastole), the elastic recoil of the arterial walls propels the blood forward, ensuring a continuous and steady flow.
Clinical Significance
Atherosclerosis is the most common and significant disease affecting arteries. It is characterized by the buildup of plaque (a mixture of fat, cholesterol, and other substances) within the arterial walls, leading to their hardening and narrowing. This can restrict blood flow and increase the risk of blood clots, which can cause heart attacks and strokes. Other arterial conditions include aneurysms, which are bulges in the arterial walls that can rupture, and peripheral artery disease, which affects the arteries in the limbs.

2. Veins: The Low-Pressure Return System
Veins are the blood vessels responsible for carrying deoxygenated blood from the body’s tissues back to the heart. They are the low-pressure counterparts to arteries and are equipped with unique features to facilitate blood flow against gravity.
Anatomy of Veins
Like arteries, veins have three layers, but they are thinner and less muscular:
•Tunica Intima: The inner layer, which includes a smooth endothelium.
•Tunica Media: The middle layer, which is much thinner than in arteries, with less smooth muscle and elastic tissue.
•Tunica Externa (Adventitia): The outer layer, which is the thickest layer in veins and provides structural support.
A key feature of veins, particularly in the limbs, is the presence of valves. These are flap-like structures that prevent the backflow of blood, ensuring that it continues to move towards the heart.
Function of Veins
The primary function of veins is to return deoxygenated blood to the heart. Because the pressure in the venous system is low, the movement of blood is assisted by the contraction of skeletal muscles surrounding the veins (the skeletal muscle pump) and the pressure changes in the chest during breathing (the respiratory pump). The valves in the veins are essential for making this system work effectively.
Clinical Significance
Common venous disorders include varicose veins, which are enlarged and twisted veins that can be seen on the skin’s surface, and deep vein thrombosis (DVT), which is the formation of a blood clot in a deep vein, usually in the legs. DVT is a serious condition because the clot can break loose and travel to the lungs, causing a life-threatening pulmonary embolism.
3. Capillaries: The Exchange Hubs
Capillaries are the smallest and most numerous blood vessels in the body, forming an extensive network that connects arterioles (small arteries) to venules (small veins). They are the crucial sites where the exchange of gases, nutrients, and waste products occurs between the blood and the body’s cells.
Anatomy of Capillaries
The most striking anatomical feature of capillaries is their extremely thin walls, typically consisting of a single layer of endothelial cells. This thinness, combined with their small diameter (often just wide enough for red blood cells to pass in single file), maximizes the efficiency of exchange processes. The total surface area of all capillaries in the body is vast, further enhancing their exchange capabilities.
Function of Capillaries
The primary function of capillaries is to facilitate the rapid and efficient exchange of substances. Oxygen and nutrients (like glucose and amino acids) diffuse from the blood in the capillaries into the surrounding interstitial fluid and then into the cells. Conversely, waste products (such as carbon dioxide and urea) diffuse from the cells, through the interstitial fluid, and into the capillary blood to be transported away for excretion. This exchange is driven by differences in concentration gradients and blood pressure.
Clinical Significance
Capillary function is vital for tissue health. Dysfunction can lead to various problems. For instance, in diabetes, prolonged high blood sugar can damage capillaries, leading to complications like diabetic retinopathy (damage to the capillaries in the eyes, potentially causing blindness) and diabetic nephropathy (damage to kidney capillaries, leading to kidney failure). Inflammation often involves increased capillary permeability, leading to fluid leakage and swelling (edema) in affected tissues. Issues with capillary integrity can also impact drug delivery and the body’s immune response.
4. The Aorta: The Body’s Main Artery
The aorta is the largest and most crucial artery in the human body. It originates directly from the left ventricle of the heart, forming an arch over the heart before descending through the chest and abdomen. It acts as the primary conduit for distributing oxygenated blood to the systemic circulation.
Anatomy of the Aorta
The aorta is a massive, elastic artery, typically about 2-3 cm in diameter. It is divided into several distinct parts:
•Ascending Aorta: Rises from the left ventricle, giving off the coronary arteries that supply the heart muscle itself.
•Aortic Arch: Curves over the top of the heart, giving rise to major arteries that supply the head, neck, and upper limbs (brachiocephalic artery, left common carotid artery, and left subclavian artery).
•Descending Thoracic Aorta: Continues downwards through the chest, supplying blood to the chest wall and organs.
•Abdominal Aorta: Passes through the diaphragm into the abdomen, where it branches to supply the abdominal organs, pelvis, and lower limbs. It eventually bifurcates into the common iliac arteries.
Its wall structure is similar to other large arteries, with a prominent tunica media rich in elastic fibers, allowing it to stretch and recoil with each heartbeat, which is vital for maintaining continuous blood flow and pressure.
Function of the Aorta
The aorta’s primary function is to receive the high-pressure, oxygenated blood ejected from the left ventricle and distribute it efficiently to all parts of the body, except the lungs. Its elasticity helps to dampen the pulsatile flow from the heart, converting it into a more continuous flow, which is essential for perfusion of peripheral tissues. This ‘Windkessel effect’ helps maintain diastolic blood pressure.
Clinical Significance
Given its critical role, conditions affecting the aorta can be life-threatening. Aortic aneurysms are localized dilations or bulges in the aortic wall, which can rupture, leading to severe internal bleeding and often death. Aortic dissection occurs when a tear in the inner layer of the aorta allows blood to flow between the layers of the wall, separating them. This is a medical emergency that can rapidly lead to organ damage or rupture. Other conditions include aortic coarctation (a congenital narrowing of the aorta) and atherosclerosis, which can affect the aorta just like other arteries, contributing to aneurysm formation and dissection.
5. Pulmonary Arteries: The Unique Arterial Path to the Lungs
The pulmonary arteries are a unique set of arteries within the circulatory system. Unlike all other arteries in the systemic circulation, which carry oxygenated blood away from the heart, the pulmonary arteries carry deoxygenated blood from the heart to the lungs.
Anatomy of Pulmonary Arteries
The main pulmonary artery (also known as the pulmonary trunk) emerges from the right ventricle of the heart. It is relatively short and quickly divides into the right and left pulmonary arteries, each extending to the corresponding lung. Within the lungs, these arteries branch into smaller arterioles and eventually into the vast capillary network surrounding the alveoli (air sacs).
Function of Pulmonary Arteries
The primary function of the pulmonary arteries is to transport deoxygenated blood from the right side of the heart to the lungs. In the lungs, this blood undergoes gas exchange: it releases carbon dioxide (a waste product) and picks up oxygen. This process is a critical component of the pulmonary circulation, which is dedicated to oxygenating the blood.
Clinical Significance
Conditions affecting the pulmonary arteries can have severe consequences for respiratory and cardiac function. Pulmonary hypertension is a serious condition characterized by abnormally high blood pressure in the pulmonary arteries, which can lead to right-sided heart failure. Pulmonary embolism (PE) occurs when a blood clot (often originating from a deep vein thrombosis in the legs) travels to the lungs and blocks one or more pulmonary arteries, impeding blood flow and gas exchange. Both conditions are life-threatening and require immediate medical attention.
6. Pulmonary Veins: The Oxygenated Return from the Lungs
The pulmonary veins are another unique set of vessels in the circulatory system. They are responsible for carrying oxygenated blood from the lungs back to the left atrium of the heart. This makes them an exception to the general rule that veins carry deoxygenated blood.
Anatomy of Pulmonary Veins
Typically, there are four pulmonary veins, two from each lung (superior and inferior pulmonary veins from the right lung, and superior and inferior pulmonary veins from the left lung). These veins merge from the capillary beds surrounding the alveoli in the lungs and converge to enter the left atrium of the heart. Their walls are relatively thin, similar to other veins, but they do not contain valves.
Function of Pulmonary Veins
The primary function of the pulmonary veins is to transport the newly oxygenated blood from the lungs back to the left side of the heart. This completes the pulmonary circulation loop, delivering oxygen-rich blood to the systemic circulation for distribution throughout the body.
Clinical Significance
Conditions affecting the pulmonary veins can impact the heart’s ability to effectively pump oxygenated blood. Pulmonary vein stenosis is a narrowing of one or more pulmonary veins, which can lead to increased pressure in the lungs, pulmonary hypertension, and eventually heart failure. Anomalous pulmonary venous return is a congenital heart defect where one or more pulmonary veins connect to the right atrium or other systemic veins instead of the left atrium, leading to a mixing of oxygenated and deoxygenated blood and potentially causing cyanosis and heart strain.
Conclusion
The intricate network of blood vessels is fundamental to the proper functioning of the human body. Arteries, veins, capillaries, the aorta, and the pulmonary arteries and veins each play a specialized and indispensable role in the circulatory system. Arteries, with their thick, elastic walls, efficiently distribute oxygenated blood under high pressure. Veins, equipped with valves, ensure the return of deoxygenated blood to the heart. Capillaries, with their remarkably thin walls, serve as the crucial sites for gas and nutrient exchange at the cellular level. The aorta stands as the body’s main artery, initiating the systemic distribution of oxygen-rich blood, while the pulmonary arteries and veins form a unique circuit dedicated to oxygenating the blood in the lungs. Understanding the distinct anatomy, functions, and clinical significance of these five main blood vessels is key to appreciating the complexity and vital importance of the cardiovascular system in maintaining life and health.





Be First to Comment